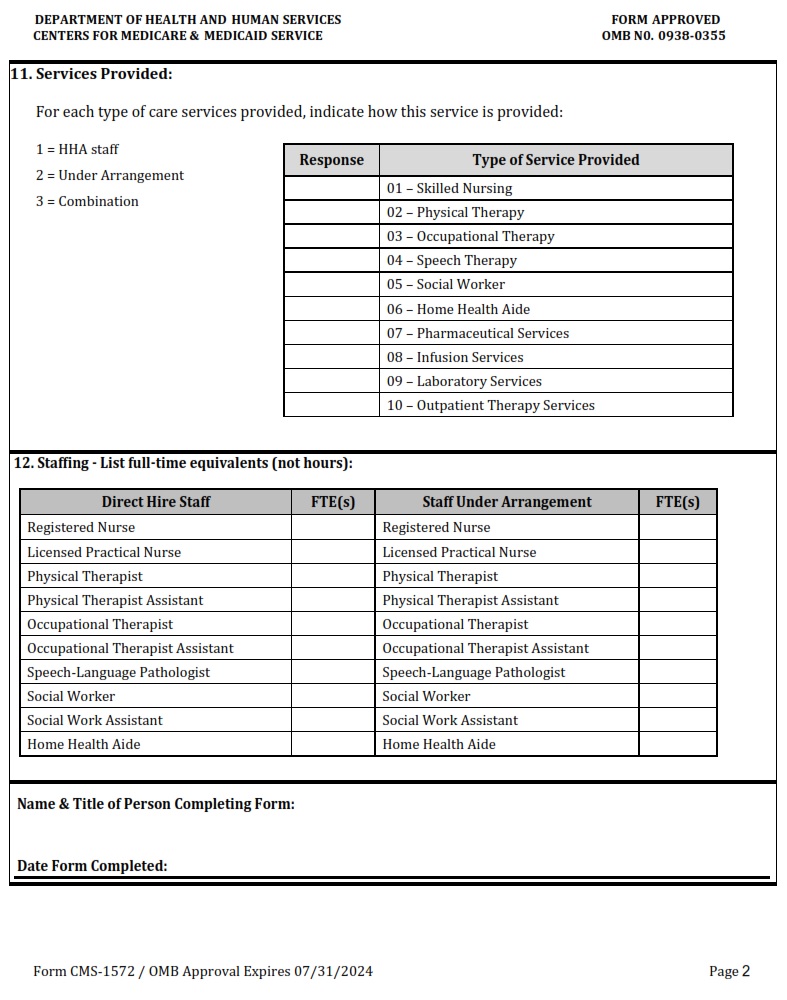
CMSFORM.ORG – CMS 417 – HOSPICE REQUEST FOR CERTIFICATION IN MEDICARE – Hospice care is a critical service for patients and their families during end-of-life stages. The ability to access hospice care through Medicare can ease the financial burden and provide peace of mind for those in need. However, it is important to understand the requirements and process for hospice certification under Medicare.
CMS 417 – Hospice Request for Certification in Medicare is a crucial form that healthcare providers must complete accurately to ensure proper reimbursement from Medicare. This article will delve into the purpose of CMS 417, its components, and how healthcare providers can successfully navigate the certification process to provide essential hospice care to their patients.
Download CMS 417 – HOSPICE REQUEST FOR CERTIFICATION IN MEDICARE
[su_table responsive=”yes”]
| Form Number | CMS 417 |
| Form Title | HOSPICE REQUEST FOR CERTIFICATION IN MEDICARE |
| Published | 2021-11-30 |
| O.M.B. | 0938-0313 |
| File Size | – KB |
[/su_table]
[download id=’1703′]
What is a CMS 417?
A CMS 417 form is a Hospice Request for Certification in Medicare. This form is used by hospice providers to request certification of a patient’s eligibility for the Medicare hospice benefit. Hospice care provides palliative care services to patients who are terminally ill and have a life expectancy of six months or less.
The CMS 417 form includes important information about the patient, such as their diagnosis, prognosis, and current treatment plan. It also requires documentation from the patient’s attending physician certifying that they meet the criteria for hospice care under Medicare guidelines.
Once completed and submitted, this form goes through an assessment process by a Medicare-certified hospice agency to determine if the patient qualifies for the coverage. If approved, the hospice provider will receive reimbursement from Medicare for services rendered until death or discharge from hospice care.
Where Can I Find a CMS 417?
If you are looking for a CMS 417 form to request certification for hospice care under Medicare, there are different avenues you can explore. One option is to visit the official website of the Centers for Medicare and Medicaid Services (CMS) and download the form from there. You can also contact your local hospice agency or Medicare Administrative Contractor (MAC) to obtain a copy of the CMS 417 form.
Another approach is to reach out to your healthcare provider or physician who can assist you in filling out the CMS 417 form accurately. They may also have a copy of the required documentation needed to support your eligibility for hospice care under Medicare. Furthermore, some healthcare facilities might have CMS 417 forms available on-site or during consultations with patients seeking hospice services.
Overall, finding a CMS 417 form should not be difficult if you know where to look. Whether through online portals, government agencies, healthcare providers, or hospice organizations – help is readily available when it comes to accessing this important document that allows patients who meet specific criteria to access end-of-life care options under their health insurance plan.
CMS 417 – HOSPICE REQUEST FOR CERTIFICATION IN MEDICARE
CMS 417 is a form that hospice agencies use to request certification in Medicare. This form requires the hospice agency to provide information about the patient’s medical condition, prognosis, and expected course of treatment. The purpose of this form is to ensure that only patients who are eligible for hospice care receive it.
To be eligible for hospice care under Medicare, a patient must have a terminal illness with an estimated life expectancy of six months or less if the disease runs its normal course. Hospice care provides comfort and support for patients nearing the end of their lives. It focuses on pain management, symptom relief, and emotional support for both the patient and their family.
Once CMS 417 is submitted by the hospice agency, Medicare will review it to determine if the patient meets eligibility requirements. If approved, Medicare will cover all costs related to hospice care including medical equipment, medications, and nursing services.